Depression, anxiety, bipolar disorder, schizophrenia. We all recognize these terms, and we all know someone struggling with some form of mental illness. According to the National Alliance on Mental Illness (NAMI), mental illness affects one in five adults in America and three-quarters of these cases begin by the age of 24. Eighteen percent of American adults live with anxiety disorders and seven percent live with depression. In fact, depression is the leading cause of disability worldwide. Despite these startling statistics, no treatment has proven 100 percent effective in treating mental illnesses, and because of a lack of consensus among medical professionals, patients are suffering.
There are a variety of causes for this lack of consensus regarding treatment. For one, there is a lack of consistency in how different clinical trials measure the success of various medications. Clinical trials attempt to quantify the severity of mental illness as a whole, but they would be more informative if they evaluated specific symptoms. It does not help that the definitions of mental illnesses tend to be broad and that the presentation of mental illness varies from patient to patient. In order to understand why diagnostic criteria are so inclusive and the impact this has on treatment, it is important to consider the history of categorizing and treating certain mental illnesses.
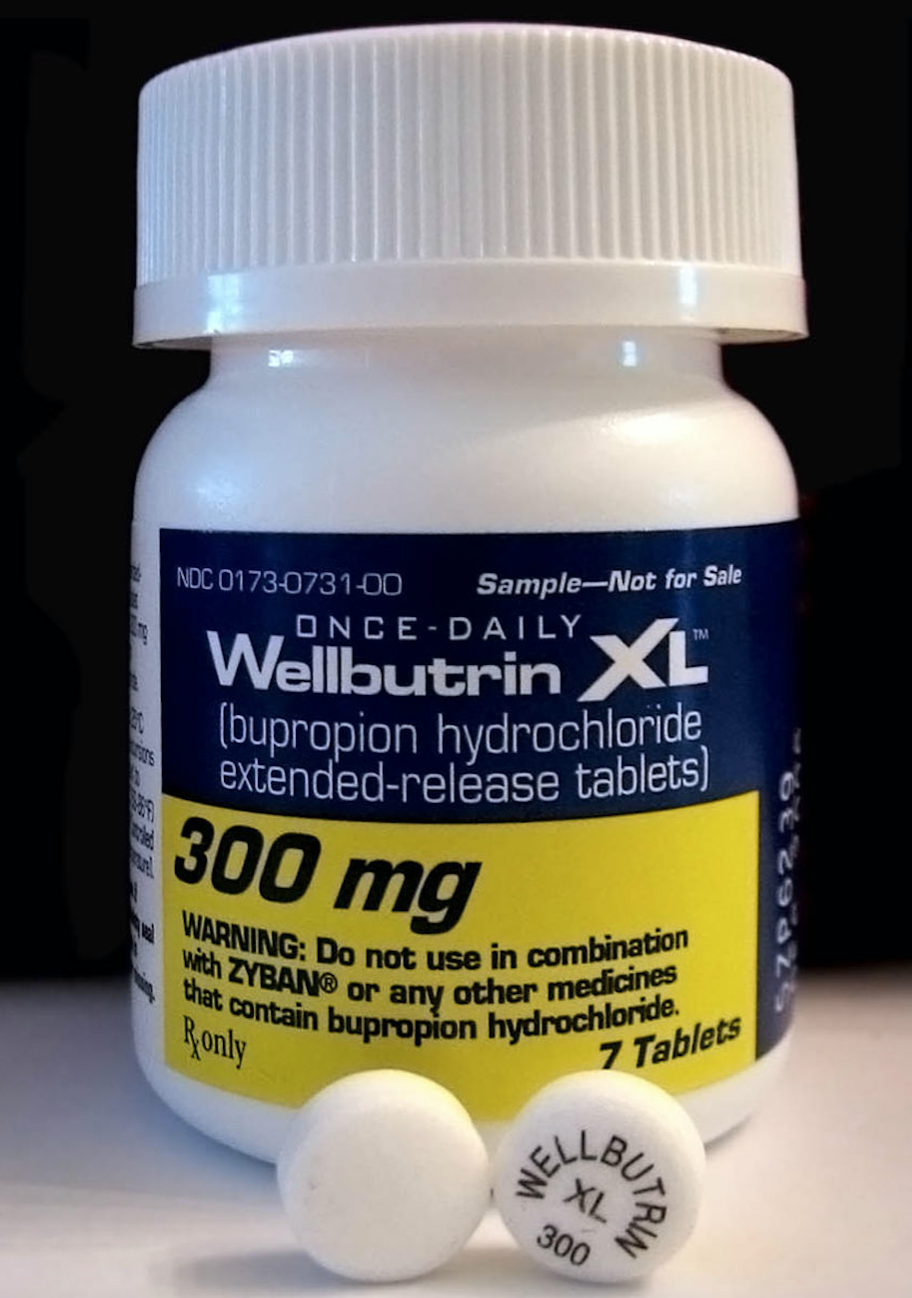
Depression medication
Ambiguity with regard to treatment of depression is particularly striking. Descriptions of depression date back millennia. The Ancient Greek physician Hippocrates described the symptoms of “melancholia,” and Sigmund Freud expanded this description in his 1917 paper Mourning and Melancholia. But it was only in 1980 that the term major depressive disorder (MDD) was added to the third edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-III). This marked a departure from the previous editions that simply made reference to “depressive reaction” or to “depressive neurosis,” and came amid increasing awareness of depression’s biological underpinnings.
Drugs developed in the 1950s were known as “tricyclics” for their three-ring structure, and although they led to improvement in 60 to 80 percent of patients, they came with severe side effects. Because of this high risk, scientists were highly motivated to seek out safer alternatives. The hypothesis that the neurotransmitter serotonin played a role in depression led to a new generation of antidepressants hitting the market. These antidepressants, known as selective serotonin reuptake inhibitors (SSRIs), had far fewer serious side effects and were massively successful.
Since the arrival of SSRIs, there have been various other classes of antidepressants developed, each associated with their own benefits and risks, ranging from weight gain and insomnia to anxiety and sexual dysfunction. With the development of these safer classes, antidepressant use increased 400 percent between 1988 and 2008. Even then, all prescription antidepressants still come marked with a black box warning—the strictest warning the FDA can give—due to the possibility of increased suicide risk.
Anxiety medication
This treatment ambiguity is also seen with regard to the treatment of anxiety. Generalized anxiety disorder (GAD) was also added to the DSM-III in 1980, having been subsumed under “anxiety neurosis” in previous editions of the manual. References to anxiety date back to Hippocrates’ descriptions of “hysteria,” but the modern conception of anxiety arose with Freud’s theory that anxiety is a physiological response to unsettling stimuli.
Prior to the shift of psychiatry to a biological model in the 1950s and 1960s, treatments for anxiety mirrored those used for depression, and many patients turned to religion, using confession, for example, to ease their anxiety. But with the revolution in drug development, doctors began marketing tranquilizers to anxiety patients. However, tranquilizers associated with dependence and severe side effects including cardiac arrest. Consequently, another class of anxiolytic drugs, the benzodiazepines (“benzos”), soon replaced tranquilizers as the prescription of choice.
Although tranquilizers and benzos directly target anxiety, it has also been shown that many classes of antidepressants, particularly SSRIs, also have antianxiety effects. This is especially important given than anxiety and depression often co-occur. However, the side-effects of antidepressants mean that these treatments are not always the best option for anxiety patients.
Alternatives to medication
Due to the potentially serious side effects, many psychiatrists advise considering non-pharmacological treatments first. These alternatives, while technically safer, are accompanied by their own advantages and disadvantages depending on the patient, further complicating the dialogue regarding optimal treatment methods. Some common alternative treatments that have been shown to be effective are talk therapy, exercise, dietary changes and yoga or meditation.

Studies have shown that in many cases, talk therapy can be just as effective as medication. Research has also demonstrated the effectiveness of lifestyle changes in treating mental illness. Cochrane, a non-government organization that compiles medical information, periodically releases reports through its Depression, Anxiety and Neurosis Review Group. According to the most recent report in 2013, when compared to psychological or pharmacological therapies, exercise is equally effective. However, patients often fail to realize that lifestyle changes such as exercise need to be treated just like medication. Too much or too little exercise or failure to establish a consistent routine can significantly reduce the benefits provided by lifestyle changes. In other words, just as with drugs, dosage and compliance matters.
Why drugs?
Both medical and sociocultural factors are important in explaining why medication tends to be the favored option. The safety profile of drugs have made huge advances over the past decades. Modern antidepressants have far fewer side effects, and modern antianxiety drugs carry a much lower risk of addiction. As such, doctors are more comfortable prescribing, and patients are more comfortable with taking these comparatively safer medications.
Media also plays a large role. Pharmaceutical giants spend billions of dollars on drug advertising, and these ads are designed to highlight the benefits while speeding through the risks. The general population sees these ads and sees miracle cures for mental health problems.
A final major consideration in the choice between medication and lifestyle change is time and money. Patients have the choice between taking a pill, which takes two seconds and costs them next to nothing thanks to modern insurance coverage, and spending hours each week exercising or hundreds of dollars on therapy sessions.
A patient-centric approach
The lack of consensus regarding the optimal treatment for mental illnesses makes it difficult to give concrete recommendations. This lack of consensus stems partially from the inconsistencies in how improvement due to any given intervention is measured. For example, previous drug company-sponsored research on medications showed that only 44 percent of antidepressant trials resulted in significant improvements in patients’ symptoms. However, a 2015 report pointed out the fact that these trials used the Hamilton Depression Rating Scale (HDRS), a 17-item scale that was developed in the 1950s and is thus rather outdated. When the team re-analyzed the data, looking for changes in only one element of the scale, depressed mood, it was shown that 91 percent of trials resulted in significant improvement.

A similar problem arises when physicians attempt to determine which treatment would be most appropriate for a given patient. “[Psychiatrists] understand that there is no unitary solution for whatever a person presents with… and it is rare that one thing works perfectly,” said Michael Sernyak, a professor of psychiatry at Yale and CEO of the Connecticut Mental Health Center. The DSM-5 lists nine symptoms of major depression, and a patient must meet five to qualify for a diagnosis. For a diagnosis of GAD, a patient must meet only three of six listed symptoms. Given the countless possible combinations of symptoms, it is clear that not all depression or anxiety is equal. As such, it makes sense that different treatments might be more effective for different patients. Very little research has been done on the effects of medications on specific symptoms, and research has shown that many patients benefit from a multifactorial approach to treatment consisting of medication, psychotherapy and lifestyle changes.
Treatments for mental illnesses are not one-size-fits-all. Each patient presents with a specific combination of symptoms and may respond to certain treatments more than others. When considering moving forward with a treatment plan, patients should be presented with all options, and physicians should tailor decisions based on the unique characteristics of each patient rather than on statistics from studies that are broad-based and thus not necessarily applicable to the patient. In other words, for the best results, doctors should always think of the patient, not the numbers.
Additional Reading: Hieronymus, F et al. (2015). Consistent superiority of selective serotonin reuptake inhibitors over placebo in reducing depressed mood in patients with major depression. Molecular Psychiatry, 21: 523-530.
About the Author: Jessica Schmerler is a senior in Jonathan Edwards College majoring in molecular, cellular & developmental biology, neuroscience track. She is a member of the Yale Journalism Initiative, a freelance writer for Scientific American MIND magazine, and Editor-in-Chief of the Yale Global Health Review. She also works in William Cafferty’s lab studying spinal cord injury.
Acknowledgments: The author would like to thank Dr. Sernyak for his time and expertise in the field of psychiatry.
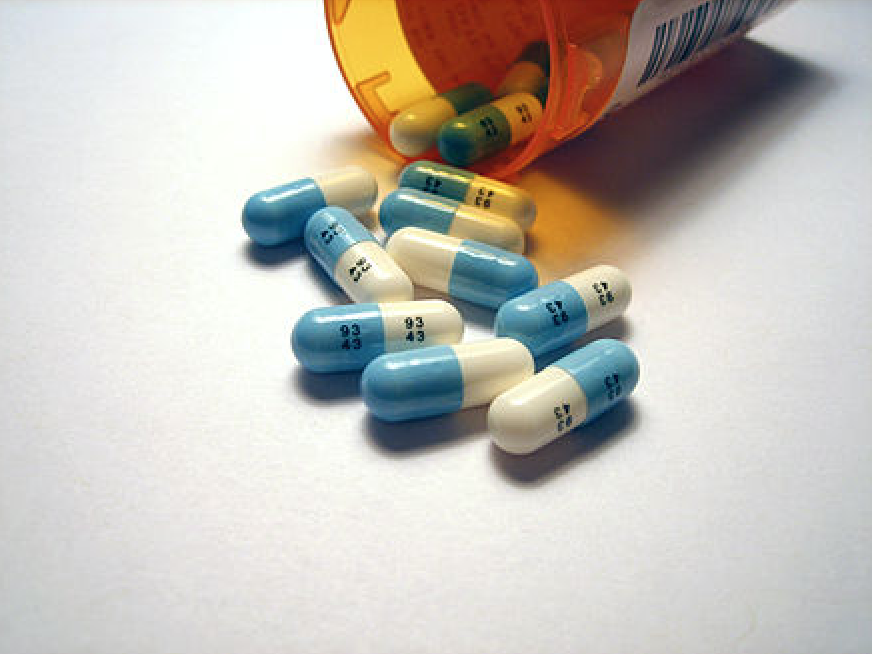
Cover image: Shown above are fluoxetine HCl (Prozac) 20mg capsules. Prozac was one of the first SSRI antidepressants and garnered significant media attention over the years. Image courtesy of Tom Varco