Research in autism medicine is seeing impressive developments at the Child Study Center of the Yale School of Medicine.
A recent study led by Dr. Pamela Ventola has improved the methods by which clinicians may analyze a patient with an Autism Spectrum Disorder (ASD) and tailor a treatment that would reduce the effects of the disorder on the patient’s social and personal life. The study sought to identify specific biomarkers in each patient that can be used to pinpoint the best possible treatment.
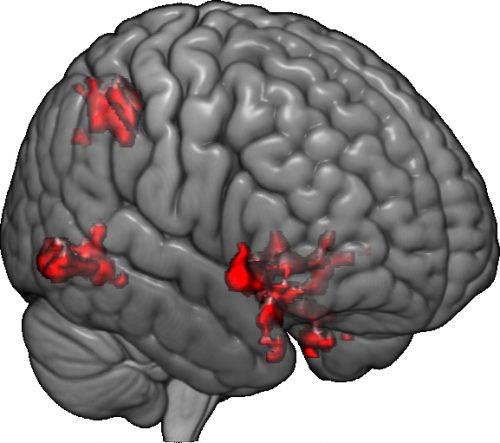
Using functional magnetic resonance imaging (fMRI) to monitor brain activity in real time for 20 ASD-afflicted children of mean age 5.9 years, Dr. Ventola and her team were able to identify neural patterns in circuits of the brain involved with “social information processing and social motivation/reward”. These patterns differed patient to patient, and these differences were compared to the patients’ response to pivotal response treatment (PRT). PRT is a naturalistic treatment approach, designed to increase the child’s social motivation.
Dr. Ventola and her team found that there was a statistically significant correlation between the distinct neurobiological patterns observed in each child and the child’s response to PRT. Those who displayed certain biomarkers were more likely to respond to PRT and reduce the social symptoms of ASD. This represents a significant development in the field of ASD treatment as it could potentially allow clinicians to personalize treatment methods.
“It is critical to have treatments and make treatments available to patients that will improve their lives” said Dr. Denis Sukhodolsky, Associate Professor at the Child Study Center and a member of Ventola’s research group. “Not having a treatment is certainly a problem, but having a treatment that is not effective for that individual patient is also a problem”.
Dr. Sukhodolsky views this study as the middle of the road for research into ASD treatment, with more developments to come. “This approach to autism treatment started 40 or 50 years ago, and it is continuously refined to be more specific to the patients,” said Dr. Sukhodolsky. Work on biomarkers is fairly new and is dependent on technology. The next step is a randomized sample that compares PRT to a control treatment to validate improvements in outcome. Once this is complete, the research team can take confidence in the distinct biomarkers to aid patients with ASD.
Dr. Ventola echoed Dr. Sukhodolsky’s notion that there is still more to come in the field of personalized ASD treatment.
“[In this study] we were able to make predictions about the patient’s response to treatment based on brain data; in our next study we would like to explore whether or not there are other ways to predict response. Are there genetic differences between patients? Are there behavioral factors that can be used? I can’t imagine that they are not there,” said Dr. Ventola.
This study represents exciting potential in the methods of ASD treatment. Dr. Ventola, Dr. Sukhodolsky, and many others at the Child Study Center are working towards a brighter future for those afflicted by the disorder.