
For many, a diagnosis of diabetes carries with it a lifelong sentence of glucose monitors and insulin injections. Although the associated technology has improved, the essential nature of treatment has not changed since the discovery and subsequent commercial production of insulin in the 1920s. However, a recent clinical study led by Dr. Kevan Herold, Yale Professor of Immunobiology and Medicine (Endocrinology), aims to improve treatments for patients with type 1 diabetes.

Type 1 Diabetes
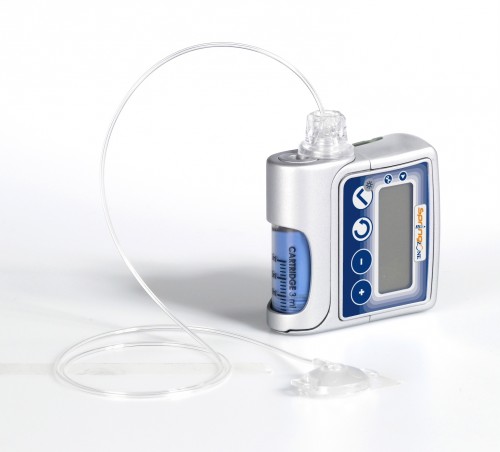
Most people are familiar with type 2 diabetes, a disease associated with poor diet and excess weight. However, type 1 diabetes is a more severe form of the illness, which is most often diagnosed in children and represents up to ten percent of all diabetes cases. In this condition, immune cells known as T cells attack insulin-producing β cells in the pancreas, which leads to decreased levels of insulin production. While a concrete cause for type 1 diabetes is unclear, there is evidence for strong genetic and environmental factors. As the disease progresses and the death of beta cells results in falling insulin levels, patients need to deliver the insulin their body cannot supply through injection or insulin pumps.
Though researchers and clinicians have expanded their knowledge of the disease in recent decades, options for treatment are still limited. Diagnosed individuals must carefully and constantly monitor their blood glucose levels, then administer insulin at several points throughout the day. Furthermore, as Herold explained, since the advent of insulin, “there has never been another treatment that fundamentally changed the natural history of the disease.” Even with appropriate management, a significant fraction of type 1 diabetes patients today develop complications that include kidney failure, blindness, and various neuropathies.

A Potential Treatment
Herold’s study may foreshadow a new treatment that could change how patients manage their condition. In a clinical trial, patients were treated with the drug Teplizumab, a monoclonal antibody which binds to a specific region of the CD3 receptor. This receptor is found on the surface of all T cells, including the ones responsible for β cell destruction in type 1 diabetes, and helps T cells recognize their target antigen. The reason that binding to the CD3 receptor reduces attacks on β cells is as of yet unknown. Unlike other CD3-targeted antibodies, Teplimuzab does not simply deplete T cells from the body. Research by Herold and Richard Flavell, Sterling Professor and Chair of Immunobiology at Yale, suggests that the drug “causes cells to migrate to the gut, where they may acquire a regulatory function,” said Herold. These induced regulatory T cells can then suppress the immune response.
In the study, two groups of patients, all of whom were within eight weeks of their initial diagnosis, were treated, either with Teplimuzab or with nothing as a control. One year later, the patients were again treated for two weeks with the same substance. Throughout these years, the patients’ insulin production and consequently β cell function were monitored by measuring levels of C-peptide, a short protein found in a precursor to insulin.
What the researchers found was extremely promising. In patients receiving the drug, the average decline in C-peptide was 75 percent less than the control group after two years, meaning their insulin production remained relatively close to constant. However, not all the treated patients responded similarly, leading to a second critical question: Why did some patients respond better than others?

Identifying Responders
To understand the answer to this question, it is important to first define responders and non-responders. According to Herold, the distinction is straightforward: “We looked at the decline in C-peptide in the control group after two years. Drug-treated subjects who had the same level of decline are non-responders, and those with less decline are responders.” Based on this criteria, of the 49 treated subjects who completed the study, 27 were non-responders and 22 were responders. Examining the C-peptide levels over time within these groups revealed that non-responders actually had similar levels of C-peptide as the control group. In patients who responded to the treatment, C-peptide levels remained at or above the initial baseline for an average of 18 months, and the level of C-peptide was almost three times higher than the control group at that time.
After discovering this drastic difference, the team was very interested in determining what caused it. “We thought for sure that there were going to be big immunologic differences, but [the distinctions] were fairly subtle,” Herold said. Rather, “the major difference seemed to be that the responders used less insulin going into the trial than the non-responders, and also had better glucose control.” While this initially seemed counterintuitive, as one might expect that responders would end up with lower blood glucose levels rather than the other way around, the team found the same trend when they reevaluated previous trials. One potential explanation is that glucose levels may affect immune responses or β cells directly. Herold’s lab is interested in investigating the links, as he believes that “there’s an interesting interrelationship between metabolic control and immunologic effects that really has not been addressed at all.”

Hope for the Future
The success of the trial has not stopped Herold from looking towards improvements and future applications. He is currently continuing to track the response of patients in the trial to see how long their C-peptide levels remain stable. He has also continued to investigate basic immunological questions about type 1 diabetes and Teplimuzab, including defining biomarkers for the disease and investigating the role of the microbiota in regulating the differentiation of regulatory T cells in the gut. By better understanding the disease pathology and interaction with the drug, more effective interventions can be developed.
In addition to these studies, Herold is enrolling patients for an even more ambitious trial which aims to prevent or delay the onset of type 1 diabetes. “We know from monitoring relatives of people with type 1 diabetes that those who have autoantibodies and altered glucose monitor tests have a greater than 75 percent risk of getting diabetes in five to seven years,” he said. “The question is, if you come in much earlier, does the drug prevent the disease altogether?” If the trial shows that Teplimuzab has an effect in preventing type 1 diabetes, it could lead to a major advance in patient care, as those at risk can currently do little to stop disease onset. Together with Herold’s other ongoing research, the study represents a long-awaited hope for improved type 1 diabetes treatments.
About the Author: Grace Cao is a sophomore Molecular, Cellular and Developmental Biology major in Timothy Dwight College. She is a Copy Editor for the Yale Scientific Magazine and works in Professor Carla Rothlin’s lab in the Immunobiology Department.
Acknowledgements: The author would like to thank Professor Herold for his time and enthusiasm in explaining his research on type 1 diabetes.
