As consumers of food, we all possess some intuition about overeating. We eat not only when we are hungry, but also when environmental cues, such as the sight or scent of a sweet treat, cause us to crave food. Even though we interact with food on a daily basis, researchers have only recently begun to understand the complexity of the pathways and structures that connect the mind and the body to the diet.
Research recently published by Rick Jenison at the University of Wisconsin, Madison, has revealed that a subset of neurons within the amygdala display activity patterns that correlate with the values that individuals assign to food items.
With the consent of three patients who were undergoing surgical therapy for epilepsy, Jenison used electrodes that had been implanted as part of the therapy to track the activity of individual neurons in the patients’ amygdalae. He presented each patient with 50 images of various junk foods, for which they could bid anywhere between $0 and $3. Jenison then demonstrated that 16 of 51 neurons that were monitored during the study exhibited either a positive or negative correlation with the bid value.
Jenison’s findings extend the conclusions of recent animal studies that certain neurons in these structures fire in response to rewards, aversive stimuli, or both. In the paper reporting this research, he speculates that the role of the amygdala in value judgment might mean that the structures are important in a number of decision-making tasks, including food choice. If this hypothesis were true, it would add value computation in the amygdala to a growing list of brain structures and processes that are known to influence our food choices.
One brain structure whose role in food consumption has long been known is the nucleus accumbens, part of the famous “reward circuit” that complements the addictive effects of substances such as cocaine. A 2003 mouse study demonstrated that a class of chemicals called μ-opioids can stimulate the nucleus accumbens and activate a network of other brain regions, including the hypothalamus and the ventral tegmental area. Activation of these areas by the neurotransmitter dopamine results in a marked increase in consumption of fatty, salty, and sweet foods.
The relationship among the brain, the body, and the diet becomes far more complex in the caudate nucleus, another region that contains dopamine-sensitive neurons. Dana Small and the Affective Sensory Neuroscience Laboratory at the John B. Pierce Laboratory have been studying this region for the past few years.
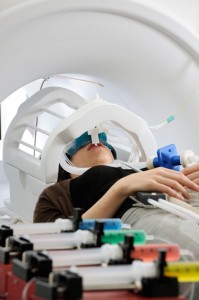
In 2008, Small and her collaborators published results of functional MRI (fMRI) studies that demonstrated a negative correlation between body weight and activation of the caudate nucleus in response to consumption of energy-rich foods. In the same paper, the team hypothesized that certain individuals may overeat because they have an allele of the TaqIA gene that reduces dopamine signaling, thus also reducing caudate nucleus activity and the sense of reward associated with food consumption.
Since then, both Small and other investigators have conducted further studies, and the results have complicated this seemingly simple relationship among food consumption, body weight, and the caudate nucleus. For example, children of healthy weight who are at genetic risk for obesity because of obese parents displayed higher caudate activity in response to energy-rich food than other children of the same weight. Indeed, the response of the caudate nucleus turned out to have no correlation with any measure of food-related reward or motivation.
“The simple idea that brought us to the table is wrong,” Small says, pointing instead to new research by Paul Johnson and Paul Kenny of Florida’s Scripps Research Institute, which suggests that changes in caudate nucleus activity might occur alongside overeating and weight gain. These results suggest that overeating may not just be a function of pre-existing brain states – overeating may actually change the brain in long-lasting ways.
In light of this new model, Small’s lab is now turning its attention to new questions. Small has several on her mind, including, “Is this caudate response related to any functional changes? Can you get it to come back up again, by losing weight? And what’s the mechanism?” These questions, along with similar queries posed by dozens of other researchers, will expand our knowledge of the brain’s response to food and help us move closer to understanding the web of processes that come into play every time we “can’t eat just one.”
