Hand tremors. Rigid muscles. Speech changes. These are symptoms typically associated with Parkinson’s disease, a brain disorder that results from an unexplained loss of dopamine producing neurons in the brain. Parkinson’s often develops around age 50, and has no known cure.
However, the chronic, degenerative disease has cognitive symptoms, in addition to the motor difficulties more commonly known by the general public. According to neurologist Dr. Nandakumar Narayanan of the University of Iowa, Parkinson’s disease interferes with the perception of time (e.g. deciding when it is safe to cross the road), a “mission critical behavior” necessary for survival. The disease also causes memory problems and difficulty in inhibiting inappropriate actions. For example, one Parkinson’s patient described by Narayanan would propose to every woman in the street. Finally, Parkinson’s also causes “executive deficit,” a lack of high-level cognitive abilities that control attention, planning, and memory.
More importantly, while there are treatments to alleviate the motor symptoms of Parkinson’s disease by temporarily boosting dopamine levels in the brain, there are “no treatments for the cognitive circuits,” says Narayanan. Furthermore, unlike with the motor symptoms, scientists do not know why Parkinson’s disease produces these cognitive symptoms. This is where Narayanan’s recent journal paper, which explores the role of prefrontal dopamine receptors, comes into play.
As a resident at Yale, Narayanan, along with his colleagues, explored the function of special dopamine receptors in the prefrontal cortex of the brain. Located in the front of the brain and before the motor cortex, the prefrontal cortex controls higher-level and goal-oriented cognitive abilities. The team built, in large part, on the work of neuroscientist Patricia Goldman-Rakic, who mapped dopamine receptors to memory functions.
The researchers in Narayanan’s study conducted experiments to test the effect of turning on and off D1 dopamine receptors on the time perception and control of rodents. First, the rodents were trained to perform a time test in which they were required to estimate the arrival of a reward every 20 seconds. Then, the team injected a virus into the rodents, one of which was encoded with a protein that inhibits the function of dopamine receptors. With this experiment, Narayanan and his colleagues found that rodents injected with the virus suffered from impaired temporal control. Furthermore, the researchers found that only D1 dopamine receptors, and not D2, were involved in temporal control.
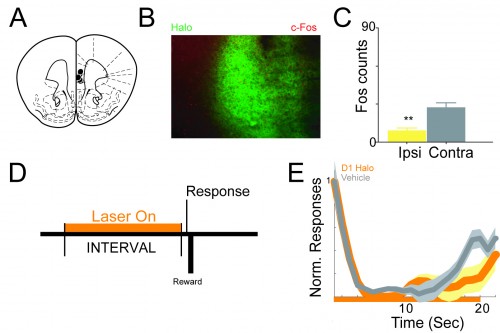
Finally, the researchers used a technique called optogenetics, in which light-sensitive genes are inserted into a specific part of the brain. In the study, these genes were put into the D1 cortex. Then, individual D1 neurons were turned on and off using laser light and a fiber optic tether. With this technology, the researchers found a direct link between prefrontal D1 receptors and temporal control. The lack of D1 receptors caused impaired temporal control, and the presence of the receptors improved the rodents’ ability to sense time.
The next step, says Narayanan, is to “map the circuitry of movement disorders in Parkinson’s disease” in his new lab. New therapy and targeted drugs that utilize the D1 pathway can then be developed to help treat the cognitive symptoms of patients with Parkinson’s disease. With Narayanan’s discovery of the link between temporal control and Parkinson’s, scientists are one step closer to decoding this mysterious disease.
