Imagine growing a heart that is an exact match for a transplant patient, a finger for someone in an accident, or a leg for veteran who lost his at war. Recent advances in the field of stem cell research may make such endeavors possible by using a patient’s own stem cells to regrow tissues or organs afflicted by disease, turning various fields of medicine towards a more personalized approach. Since the 2012 Nobel Prize awarded to John B. Gurdon and Shinya Yamanaka “for the discovery that mature cells can be reprogrammed to become pluripotent,” stem cell research has been flourishing. Recently, Japanese scientists took a major stride forward when they successfully converting blood cells back to pluripotent embryonic stem cells by treating them with an acid bath.
The novelty of this study derives from the development of a simple, noninvasive approach to induce mature cells to become pluripotent stem cells. Unlike previous techniques, this newly discovered phenomenon, known as stimulus-triggered acquisition of pluripotency (STAP), requires neither transfer of DNA from one cell to another nor the introduction of specific DNA-binding proteins. The Japanese research team, headed by Dr. Haruko Obokata of the RIKEN Center for Developmental Biology in Japan in collaboration with Dr. Charles Vacanti at Brigham & Women’s Hospital in Boston, accomplished the feat using blood cells from mouse spleens. They are now trying to replicate the results using human blood cells.

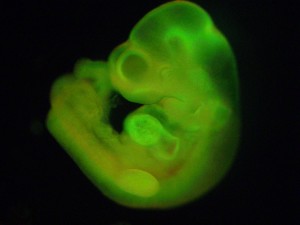
The inception of this unique approach arose from Obokata’s curiosity when she noticed that blood cells shrank to a size resembling stem cells after being squeezed through a capillary tube. Banking on the hypothesis that stress was inducing such changes, Obokata discovered that stresses in the form of acidic solutions and physical squeezing induced cells to behave like stem cells. To test that these stress-altered cells were indeed pluripotent, the cells were fluorescently tagged and injected into mice embryos. In the resulting developing pups, fluorescence was observed in all differentiated cell types, indicating that the fluorescently tagged stress-induced cells were indeed capable of differentiating into any cell type. Vacanti stated in an interview with CNN that this change induced by environmental stimuli is a “natural process that cells normally respond to.”

The simple and groundbreaking nature of this study has the research world buzzing with excitement. Chris Mason, a professor of regenerative medicine at University College of London, elaborated to the New York Times: “I thought — ‘my God that’s a game changer!’ … If this works in people as well as it does in mice, it looks faster, cheaper and possibly safer than other cell reprogramming technologies — personalized reprogrammed cell therapies may now be viable.”
With each discovery in stem cell pluripotency, researchers advance towards simplicity and efficiency. Jeff Karp, an associate professor at Brigham & Women’s Hospital in Boston, told CNN that the new method could produce stem cells up to ten times faster than current methods. Further research is still necessary before this technique can be used in humans, as the researchers still have not worked out the cellular mechanisms by which stress caused blood cells to change. Yet, a bright future lies ahead for stem cell research, a field which has been growing at “lightning speed” according to Karp. If the methods translate well to research in human cells, this finding will dramatically accelerate the progress towards better, safer personalized medicine.
Editor’s Note: Since its January 30 publication date, the claims in Obokata’s paper have been called into question. According to the RIKEN Center for Developmental Biology, the case is still under investigation. In an interview with Knoepfler, Wakayama asked for a wait period of “at least one year” to determine whether the technique could be replicated.
